- Doctor Dr Deepak Vaidya
- Surgery Glaucoma Treatment
- Date April 27, 2018
What is Glaucoma?
Glaucoma is a slow, progressive condition resulting in the loss of vision due to high intraocular pressure. Dr. Vaidya Eye Hospital provides excellent Glaucoma Treatment in Mumbai.
Glaucoma is a disease of the optic nerve. It is the world’s second leading cause of blindness. While it might not be curable, it is preventable This is if it is diagnosed at an early stage. Regular eye tests and check-ups help in detecting it.
It is an eye condition that causes loss of vision. This occurs due to increased pressure within the eyeball that, in turn, damages the optic nerve. The optic nerve carries images formed on the retina, to the brain. Any damage to it, thus, results in damage to sight. Since Glaucoma can cause blindness without symptoms, it is often called the ‘sneak thief of sight’.

Types of Glaucoma:
Chronic Open-Angle Glaucoma –
This is the most common type of Glaucoma. It usually occurs over the age of 45. Because there is resistance to the outflow of fluid in the eye which causes a rise in the Intraocular Pressure. It develops gradually without having obvious symptoms. The patient may lose vision, starting from peripheral vision, leaving only central or ‘tunnel’ vision.
Acute (Angle Closure) Glaucoma –
It happens due to a block of the flow of fluid in the eye. It causes a sudden rise in eye pressure and requires immediate treatment. The symptoms are severe pain in the eye, headache, nausea, reduced vision, and seeing rainbow coloured rings around lights.
Chronic Angle Closure glaucoma –
This occurs when the ‘drainage’ canal of the eye is closed by the iris. It almost behaves like open angle Glaucoma.
Developmental Glaucoma –
It is a variety of angle closure Glaucoma. It can be divided into congenital glaucoma (occurs in infants from the time of birth) and juvenile glaucoma (occurs in children and young adults).
Normal Tension Glaucoma –
This is a form of open angle Glaucoma. Here, due to the excessive sensitivity of the optic nerve to normal levels of eye pressure, the patient gradually loses their vision. Therefore, regular eye check-ups are necessary: to examine the changes in the optic nerve.
Secondary Glaucoma –
Certain diseases and conditions damage the eye’s drainage system. These are diseases like diabetes, arthritis, cataract, eye injuries or inflammation of the eye, steroid drug use for a long time, and eye tumors. Having any of these diseases increases the susceptibility of one to developing Glaucoma.
Get effective Glaucoma treatment in Mumbai. Call 9004496621 to schedule an appointment at Dr. Vaidya Eye Hospital and safeguard your vision
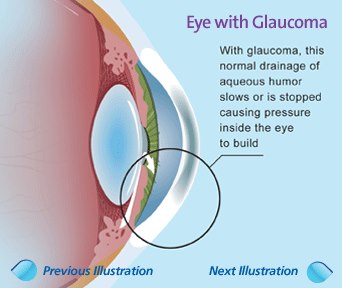
Causes of Glaucoma
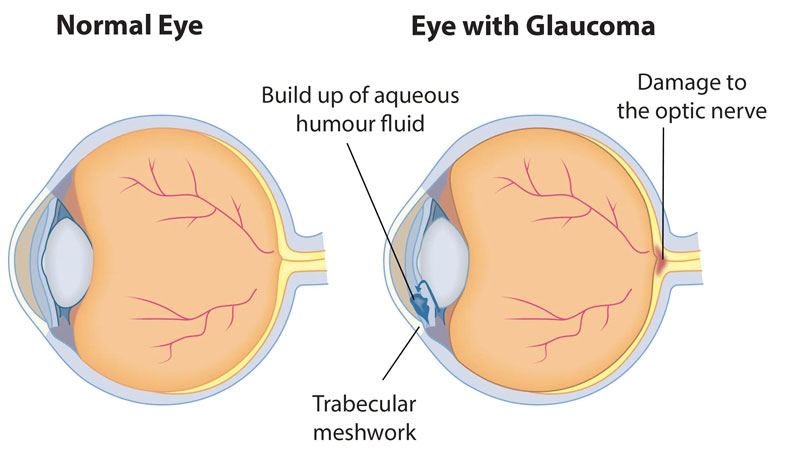
Our eyes constantly produce a clear fluid called aqueous humour. It flows through the pupil and behind the cornea. After which it drains out of the eye through a trabecular meshwork or a ‘drainage canal’. For people with Glaucoma, the fluid does not drain out freely. Which then increases eye pressure or intraocular pressure (IOP).
The optic nerve is responsible for carrying images from the retina to the brain. Raised IOP damages the optic disc and nerve fibers essential for vision.
Usually, Glaucoma affects peripheral vision. In later stages, it may cause “tunnel vision.”
Who is at risk?
- Age-Those above 40 years of age
- People with a family history of glaucoma
- Those who use steroids for long durations
- People who see coloured rings around lights
- People with diabetes or hypertension
- Any eye injuries
Tests Performed to Diagnose Glaucoma
 Tonometry
Tonometry
It is performed to measure pressure in the eye by the Applanation Tonometer. It is attached to a slit lamp. There also exists a handheld version of the same. Non-contact air puff instruments are good for screening. But they cannot be used for diagnosis of Glaucoma.
The average eye pressure is about 18 mm Hg. Remember, higher-than-average eye pressure doesn’t always mean you have Glaucoma.
Ophthalmoscopy
For this procedure, a few medicated drops are put into the eye. This is to dilate the pupil. It examines the optic disc and the back of the eye, the retina. To have a stereoscopic view, one can use a 72-D lens. A computerized scan of the optic disc can also be done.
 Optical coherence tomography (OCT)
Optical coherence tomography (OCT)
is a very useful Instrument when a patient is either a glaucoma suspect or early-to-moderate disease It also helps to detect damage and progression of optic nerve fibre.OCT gives a wealth of data to work upon, it can provide structural information about many parts of the Retina Optic nerve head & Lamina cribrosa.
In addition, a newer technology called OCT angiography, or OCTA, which helps to map the blood vessels in the retina, might also turn out to be helpful in an advanced stage of Glaucoma.
Gonioscopy
After numbing the eye, Examination of the angle of the eye is done with the help of a Gonioscope.
A special lens is gently placed on the surface of the eye. Gonioscopy allows a more accurate diagnosis of the type of glaucoma.
Pachymetry
It is done to measure the thickness of the cornea. Thickness of the cornea can increase efforts in reading and other such activities. It also, then, increases the risk of having Glaucoma.
 Perimetry
Perimetry
To confirm the diagnosis, a test is conducted on automated perimetry to know the damage of the optic nerve. In its early stages, glaucoma can only be detected or monitored by using an automated perimetry test.
An average person has a normal full-field vision, while a person with Glaucoma has areas that are not visible in the field of vision. Sometimes a diagnosis may not be possible in one visit. Therefore, periodic examinations are essential to check the progression of Glaucoma.
Treatment
Glaucoma can be controlled with treatment, but it cannot be cured. The aim is to lower the eye pressure and prevent further damage to the optic nerve and vision loss.
TREATMENT WITH EYE DROPS
There are many medicines to treat glaucoma. These drugs lower the eye pressure. Often, people with glaucoma must take these medicines for life to control it.
TABLETS
Tablets of acetazolamide -Diamox may be given to patients. It helps in reducing the amount of aqueous humour produced within
the eye.
LASER TREATMENT
Lasers are a common way of controlling Glaucoma. These Surgical laser procedures are:
Argon Laser Trabeculoplasty (ALT)
This is commonly used for open-angle Glaucoma. The laser treats the trabecular meshwork of the eye. It, in turn, increases the drainage outflow, thereby lowering the IOP. In many cases, medication is still needed.
Usually, half the trabecular meshwork is treated first. If necessary, the other half is treated as a separate procedure. This method decreases the risk of increased eye pressure following the surgery. Argon laser trabeculoplasty has, successfully, lowered eye pressure in up to 75 per cent of patients treated. This type of laser can be performed only two to three times in each eye over a lifetime.
Laser Peripheral Iridotomy (LPI)
It is used for angle-closure Glaucoma. It makes an opening through the iris, allowing aqueous fluid to flow from behind the iris directly to the interior chamber of the eye. This allows the fluid to bypass its normal route. LPI is the preferred method for managing a wide variety of angle-closure Glaucoma. This laser is most often used to treat an anatomically narrow angle and prevent angle-closure Glaucoma attacks.
Cyclophotocoagulation and ECP
These are two laser procedures for open-angle Glaucoma. They involve reducing the amount of aqueous humour in the eye by destroying a part of the ciliary body. These treatments are usually reserved for use in eyes that either has elevated IOP after having failed other more traditional treatments, or those in which filtering surgery is not possible. Transscleral cyclophotocoagulation uses a laser to direct energy through the outer sclera of the eye. It then reaches and destroys portions of the ciliary body, without causing damage to the overlying tissues. With endoscopic cyclophotocoagulation (ECP), the instrument is placed inside the eye through a surgical incision. This is to ensure that the laser energy is applied directly to the ciliary body tissues.
Incisional glaucoma surgery
Glaucoma surgery is performed as an outpatient procedure. It is usually performed with local anaesthesia, and with or without intravenous sedation. The surgery is performed under an operating microscope.
After the surgery, patients can wear their glasses and usually wear a protective shield only at bedtime for one to two weeks. The most commonly performed glaucoma incisional surgery, trabeculectomy, creates an alternative channel to divert aqueous fluid from the eye. This surgical procedure usually takes about 25-35 minutes. Glaucoma surgery often reduces or eliminates the need for future glaucoma medications in the operated eye. For some patients, the ones more at a risk of scarring, the surgeon may use an anti-fibrosing medication such as 5-fluorouracil or mitomycin C.
Can a person become blind from glaucoma?
This highly depends on the stage when it got diagnosed. If one gets diagnosed with Glaucoma at an early stage, it reduces the chances. It doesn’t necessarily mean it cannot happen. It means that it can get treated with medicines or surgeries to stabilize it. This is why regular check-ups are recommended.
Get exceptional Glaucoma Treatment in Mumbai. Call 9004496621 to schedule a consultation at Dr. Vaidya Eye Hospital and protect your vision today.
Book An Appointment
Fill out the form below and one of our representatives will get in touch with you soon!
